Hope & Health
Articles and Updates from WVU Medicine Golisano Children's
01/3/2024 | Federico Seifarth, MD, FAAP, FACS
Chest Wall Surgery: A Physical and Mental Quality of Life Treatment
WVU Medicine Children’s offers care for children and teens with various chest wall deformities. The two most common types are pectus carinatum (pigeon or raised chest) and pectus excavatum (also known as sunken or funnel chest).
What is Pectus Excavatum?
Pectus excavatum is a condition characterized by depression of the sternum (breastbone). It produces a caved-in chest, commonly referred to as “funnel chest” or “sunken chest.”
Pectus excavatum is a chest wall deformity from birth affecting an estimated one-in-400 babies. It is three-to-five times more common in males than females.
The depth and shape of the depression determine the degree of heart or lung compression.
Pectus excavatum tends to become more pronounced during the growth spurt before and during puberty. This is also the time when symptoms like shortness of breath, a fast heartbeat, or pain can arise. Some patients complain of decreased exercise tolerance.
It is well known that most affected patients suffer from poor body image, which can have a major impact on their self-esteem as well as their social and emotional development.
How is Pectus Excavatum Treated?
Historically, surgical chest wall correction required a large incision with removal and/or fracture of several ribs and the sternum (breastbone).
In 1986, Donald Nuss, MD, developed a minimally invasive repair technique of the sunken chest involving a metal implant. The principle of the minimally invasive repair is the introduction of a steel or titanium bar into the chest, pushing the sternum out and correcting the depression. This “Nuss” or “pectus bar” is individually bent during the operation or prefabricated and inserted via small incisions on the sides of the chest. The bar is advanced under the skin and breast tissue and carefully advanced across the chest under visualization with a small camera. The corrective effect is immediate, like pushing out a dent of a car. Deeper or wider depressions and older teenagers frequently require two bars.
The Nuss procedure is a minimally invasive surgical option for patients who suffer from symptoms like shortness of breath and exercise intolerance or pain, but also for patients whose psychological development is at risk. That’s why the consideration for surgical repair includes both physiologic and psychological aspects.
The depth and severity of pectus excavatum is assessed with a CT scan. The “Haller” or “pectus index” is commonly used to classify the severity of the deformity. The index is the ratio of the chest width to the shortest distance between the vertebra and sternum. A Haller index greater than 3.25 is considered an indication for surgery.
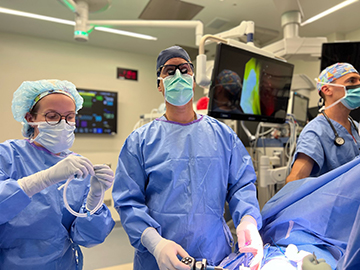
What is Chest Wall Surgery Like?
The surgery involves a large team that includes:
- Two surgeons (one on each side)
- Two surgical assistants
- One surgical technician (handing instruments)
- One anesthesiologist
- One or two operating room nurses
During the procedure, patients are under general anesthesia and fully monitored.
At the beginning, the nerves conducting the pain are numbed by applying a cold probe. This is called cryotherapy and significantly reduces the need for pain medication after the minimally invasive Nuss procedure. As a result of the cryotherapy, patients will experience numbness around the bar lasting about three-to-four months.
Not every patient with pectus excavatum requires surgical therapy. Alternatives of the Nuss procedure include observation, physical therapy, and the vacuum bell.
What is Pectus Carinatum?
Pectus carinatum, also called pigeon chest, is a deformity of the breastbone and ribs that causes the chest to stick out. It is less common than pectus excavatum.
This condition can be present at birth. Chest wall deformities run in families, but the cause for pectus carinatum and excavatum is not known.
Some children with pectus carinatum suffer from pain, shortness of breath, or exercise intolerance. In many cases, chest wall deformities become more pronounced shortly before and during puberty.
As with pectus excavatum, children with pectus carinatum suffer psychologically from their appearance. Some patients experience embarrassment and lack of self-esteem leading to social isolation and withdrawal from school and athletic involvement.
How is Pectus Carinatum Treated?
Many children with a mild chest protrusion do not require therapy.
Thankfully, there is a successful noninvasive treatment for those who need or want correction of their chest – the bracing therapy.
Surgical correction would involve a procedure under general anesthesia during which an incision is made in the mid-chest to remove abnormal ribs and reshape the sternum.
Bracing is a good alternative to surgery for many patients, but it requires a long-term commitment. Teenagers must agree to wear a brace every day for up to one year.
Prior to starting the therapy, the chest of a patient is scanned with a 3D scanner. Based on these exact measurements, a customized, individual brace is fabricated for each patient. The brace is made of a metal belt and memory foam-cushioned compression zones on the front and back. It should be worn as much as possible to apply constant pressure on the protruding chest. The brace can be removed for bathing, showering, and sports.
During the bracing therapy, the chest will be reshaped by the constant pressure from the compression pads on the front and back sides.
Initially, the brace needs to be worn day and night. After six-to-eight weeks, the brace can be taken off for few hours a day. After three-to-four months, the brace can only be worn at night. After 30 weeks, the initial treatment phase is complete, and patients might be recommended to wear the brace a few nights a week to retain the result.
Why Choose WVU Medicine Children’s for Chest Wall Treatment?
At WVU Medicine Children’s, we tailor a treatment to your child’s needs.
Our chest wall team with a dedicated nurse practitioner and staff surgeon will discuss all treatment options and guide you through the treatment process.
Follow ups can be in-person but can be conducted with an advanced practice provider at one of our satellite clinics around the state and region. You also see your provider and receive world-class care from the comfort of your home via the MyChart app.
Call 855-WVU-CARE (855-988-2273) to make an appointment today or learn more about pediatric surgical services by clicking here.
